Achilles Tendon Rupture The Facts
Overview  The Achilles tendon runs from the calf muscles at the back of the lower leg and inserts at the back of the heel. A torn achilles can be a partial rupture or a total rupture. A total rupture is more common in men affecting them 10 times more than women. Injury typically occurs 30 to 40 minutes into a period of exercise rather than at the start of a session and nearly always happens from a sudden explosive movement or bending the foot upwards. Many patients are able to continue to function following an achilles rupture due to other muscles compensating although the injured leg will be significantly weaker. There are four key tests which can help diagnose a ruptured achilles tendon. Causes The Achilles tendon can grow weak and thin with age and lack of use. Then it becomes prone to injury or rupture. Achilles tendon rupture is more common in those with preexisting tendinitis of the Achilles tendon. Certain illnesses (such as arthritis and diabetes) and medications (such as corticosteroids and some antibiotics, including quinolones such as levofloxacin [Levaquin] and ciprofloxacin [Cipro]) can also increase the risk of rupture. Rupture most commonly occurs in the middle-aged male athlete (the weekend warrior who is engaging in a pickup game of basketball, for example). Injury often occurs during recreational sports that require bursts of jumping, pivoting, and running. Most often these are tennis, racquetball, basketball, and badminton. The injury can happen in the following situations. You make a forceful push-off with your foot while your knee is straightened by the powerful thigh muscles. One example might be starting a foot race or jumping. You suddenly trip or stumble, and your foot is thrust in front to break a fall, forcefully overstretching the tendon. You fall from a significant height or abruptly step into a hole or off of a curb. Symptoms The most common initial symptom of Achilles tendon rupture is a sudden snap at the back of the heels with intense pain. Immediately after the rupture, the majority of individuals will have difficult walking. Some individuals may have had previous complains of calf or heel pain, suggesting prior tendon inflammation or irritation. Immediately after an Achilles tendon rupture, most individuals will develop a limp. In addition, when the ankle is moved, the patient will complain of pain. In all cases, the affected ankle will have no strength. Once the Achilles tendon is ruptured, the individual will not be able to run, climb up the stairs, or stand on his toes. The ruptured Achilles tendon prevents the power from the calf muscles to move the heel. Whenever the diagnosis is missed, the recovery is often prolonged. Bruising and swelling around the calf and ankle occur. Achilles tendon rupture is frequent in elderly individuals who have a sedentary lifestyle and suddenly become active. In these individuals, the tendon is not strong and the muscles are deconditioned, making recovery more difficult. Achilles tendon rupture has been reported after injection of corticosteroids around the heel bone or attachment of the tendon. The fluoroquinolone class of antibiotics (such as ciprofloxacin [Cipro]) is also known to cause Achilles tendon weakness and rupture, especially in young children. Some individuals have had a prior tendon rupture that was managed conservatively. In such cases, recurrence of rupture is very high. Diagnosis To diagnose an Achilles tendon injury, your health care provider will give you a thorough physical exam. He or she may want to see you walk or run to look for problems that might have contributed to your Achilles tendon injury. Non Surgical Treatment Non-operative treatment consists of placing the foot in a downward position [equinus] and providing relative immobilization of the foot in this position until the Achilles has healed. This typically involves some type of stable bracing or relative immobilization for 6 weeks, often with limited or no weight bearing. The patient can then be transitioned to a boot with a heel lift and then gradually increase their activity level within the boot. It is very important that the status of the Achilles is monitored throughout non-operative treatment. This can be done by examination or via ultrasound. If there is evidence of gapping or non-healing, surgery may need to be considered. Formal protocols have been developed to help optimize non-operative treatments and excellent results have been reported with these protocols. The focus of these treatments is to ensure that the Achilles rupture is in continuity and is healing in a satisfactory manner. The primary advantage of non-operative treatment is that without an incision in this area, there are no problems with wound healing or infection. Wound infection following Achilles tendon surgery can be a devastating complication and therefore, for many patients, non-operative treatment should be contemplated. The main disadvantage of non-operative treatment is that the recovery is probably slower. On average, the main checkpoints of recovery occur 3-4 weeks quicker with operative treatment than with non-operative treatment. In addition, the re-rupture rate appears to be higher with some non-operative treatments. Re-rupture typically occurs 8-18 months after the original injury.
The Achilles tendon runs from the calf muscles at the back of the lower leg and inserts at the back of the heel. A torn achilles can be a partial rupture or a total rupture. A total rupture is more common in men affecting them 10 times more than women. Injury typically occurs 30 to 40 minutes into a period of exercise rather than at the start of a session and nearly always happens from a sudden explosive movement or bending the foot upwards. Many patients are able to continue to function following an achilles rupture due to other muscles compensating although the injured leg will be significantly weaker. There are four key tests which can help diagnose a ruptured achilles tendon. Causes The Achilles tendon can grow weak and thin with age and lack of use. Then it becomes prone to injury or rupture. Achilles tendon rupture is more common in those with preexisting tendinitis of the Achilles tendon. Certain illnesses (such as arthritis and diabetes) and medications (such as corticosteroids and some antibiotics, including quinolones such as levofloxacin [Levaquin] and ciprofloxacin [Cipro]) can also increase the risk of rupture. Rupture most commonly occurs in the middle-aged male athlete (the weekend warrior who is engaging in a pickup game of basketball, for example). Injury often occurs during recreational sports that require bursts of jumping, pivoting, and running. Most often these are tennis, racquetball, basketball, and badminton. The injury can happen in the following situations. You make a forceful push-off with your foot while your knee is straightened by the powerful thigh muscles. One example might be starting a foot race or jumping. You suddenly trip or stumble, and your foot is thrust in front to break a fall, forcefully overstretching the tendon. You fall from a significant height or abruptly step into a hole or off of a curb. Symptoms The most common initial symptom of Achilles tendon rupture is a sudden snap at the back of the heels with intense pain. Immediately after the rupture, the majority of individuals will have difficult walking. Some individuals may have had previous complains of calf or heel pain, suggesting prior tendon inflammation or irritation. Immediately after an Achilles tendon rupture, most individuals will develop a limp. In addition, when the ankle is moved, the patient will complain of pain. In all cases, the affected ankle will have no strength. Once the Achilles tendon is ruptured, the individual will not be able to run, climb up the stairs, or stand on his toes. The ruptured Achilles tendon prevents the power from the calf muscles to move the heel. Whenever the diagnosis is missed, the recovery is often prolonged. Bruising and swelling around the calf and ankle occur. Achilles tendon rupture is frequent in elderly individuals who have a sedentary lifestyle and suddenly become active. In these individuals, the tendon is not strong and the muscles are deconditioned, making recovery more difficult. Achilles tendon rupture has been reported after injection of corticosteroids around the heel bone or attachment of the tendon. The fluoroquinolone class of antibiotics (such as ciprofloxacin [Cipro]) is also known to cause Achilles tendon weakness and rupture, especially in young children. Some individuals have had a prior tendon rupture that was managed conservatively. In such cases, recurrence of rupture is very high. Diagnosis To diagnose an Achilles tendon injury, your health care provider will give you a thorough physical exam. He or she may want to see you walk or run to look for problems that might have contributed to your Achilles tendon injury. Non Surgical Treatment Non-operative treatment consists of placing the foot in a downward position [equinus] and providing relative immobilization of the foot in this position until the Achilles has healed. This typically involves some type of stable bracing or relative immobilization for 6 weeks, often with limited or no weight bearing. The patient can then be transitioned to a boot with a heel lift and then gradually increase their activity level within the boot. It is very important that the status of the Achilles is monitored throughout non-operative treatment. This can be done by examination or via ultrasound. If there is evidence of gapping or non-healing, surgery may need to be considered. Formal protocols have been developed to help optimize non-operative treatments and excellent results have been reported with these protocols. The focus of these treatments is to ensure that the Achilles rupture is in continuity and is healing in a satisfactory manner. The primary advantage of non-operative treatment is that without an incision in this area, there are no problems with wound healing or infection. Wound infection following Achilles tendon surgery can be a devastating complication and therefore, for many patients, non-operative treatment should be contemplated. The main disadvantage of non-operative treatment is that the recovery is probably slower. On average, the main checkpoints of recovery occur 3-4 weeks quicker with operative treatment than with non-operative treatment. In addition, the re-rupture rate appears to be higher with some non-operative treatments. Re-rupture typically occurs 8-18 months after the original injury. 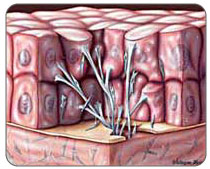 Surgical Treatment Debate remains regarding the best form of treatment for a ruptured Achilles tendon. The 2 options are:immobilisation or operation. A recent meta-analysis of scientific studies showed that compared to immobilisation, an operation reduces the risk of re-rupture and allows a quicker return to work. An operation is not without risk and these must be balanced against the benefit of a lower re-rupture rate. Both treatments involve immobilisation for 8 weeks. Prevention To help prevent an Achilles tendon injury, it is a good practice to perform stretching and warm-up exercises before any participating in any activities. Gradually increase the intensity and length of time of activity. Muscle conditioning may help to strengthen the muscles in the body.
Surgical Treatment Debate remains regarding the best form of treatment for a ruptured Achilles tendon. The 2 options are:immobilisation or operation. A recent meta-analysis of scientific studies showed that compared to immobilisation, an operation reduces the risk of re-rupture and allows a quicker return to work. An operation is not without risk and these must be balanced against the benefit of a lower re-rupture rate. Both treatments involve immobilisation for 8 weeks. Prevention To help prevent an Achilles tendon injury, it is a good practice to perform stretching and warm-up exercises before any participating in any activities. Gradually increase the intensity and length of time of activity. Muscle conditioning may help to strengthen the muscles in the body.
Achilles Tendon Pain High Arches
 This nagging injury can be long-lasting if not treated - and if your running form needs some work. The name Achilles is said to be a combination of two Greek words that together mean ?grief of the people.? The injury that bears that hero?s name, in honor of his only weakness, certainly aggrieves many runners, with Achilles tendinitis accounting for around 10 percent of running injuries. Technically, Achilles tendinitis is acute inflammation of the tendon that runs along the back of the ankle. Pain in that area for longer than a couple weeks is not really tendinitis anymore. Athletes, however, tend to characterize any pain along the tendon above the back of the heel as Achilles tendinitis. Achilles tendinitis can be confused with other injuries, such as heel problems, but the hallmark sign is if you?re pinching the Achilles and it?s really sore.
This nagging injury can be long-lasting if not treated - and if your running form needs some work. The name Achilles is said to be a combination of two Greek words that together mean ?grief of the people.? The injury that bears that hero?s name, in honor of his only weakness, certainly aggrieves many runners, with Achilles tendinitis accounting for around 10 percent of running injuries. Technically, Achilles tendinitis is acute inflammation of the tendon that runs along the back of the ankle. Pain in that area for longer than a couple weeks is not really tendinitis anymore. Athletes, however, tend to characterize any pain along the tendon above the back of the heel as Achilles tendinitis. Achilles tendinitis can be confused with other injuries, such as heel problems, but the hallmark sign is if you?re pinching the Achilles and it?s really sore.
Causes
Achilles tendinitis is caused by repeated stress to the tendon, not a direct injury. Often times, this can happen from doing too much too soon and not giving your body enough time to rest or adjust to the increase in intensity or amount of exercise. Another contributing factor can be tight calf muscles. Having tight calf muscles and starting an activity can put added stress on the achilles tendon.
Symptoms
Common symptoms of Achilles tendinitis include, pain and stiffness along the Achilles tendon in the morning, pain along the tendon or back of the heel that worsens with activity, Severe pain the day after exercising, thickening of the tendon, bone spur (insertional tendinitis) swelling that is present all the time and gets worse throughout the day with activity, If you have experienced a sudden "pop" in the back of your calf or heel, you may have ruptured (torn) your Achilles tendon. See your doctor immediately if you think you may have torn your tendon.
Diagnosis
A doctor examines the patient, checking for pain and swelling along the posterior of the leg. The doctor interviews the patient regarding the onset, history, and description of pain and weakness. The muscles, tissues, bones, and blood vessels may be evaluated with imaging studies, such as X-ray, ultrasound, or MRI.
Nonsurgical Treatment
The recommended treatment for Achilles tendinitis consists of icing, gentle stretching, and modifying or limiting activity. Nonsteroidal anti-inflammatory medications (NSAIDs), such as ibuprofen or aspirin, can reduce pain and swelling. Physical therapy and the use of an orthotic (heel lift) can also be helpful. For chronic cases where tendinosis is evident and other methods of treatment have failed, surgery may be recommended to remove and repair the damaged tissue.

Surgical Treatment
There are two types of Achilles repair surgery for tendonitis (inflammation of the Achilles Tendon), if nonsurgical treatments aren't effective. Gastrocnemius recession - The orthopaedic surgeon lengthens the calf muscles to reduce stress on your Achilles tendon. D?bridement and repair - During this procedure, the surgeon removes the damaged part of the Achilles tendon and repairs the remaining tendon with sutures or stitches. Debridement is done when the tendon has less than 50% damage.
Prevention
Warm up slowly by running at least one minute per mile slower than your usual pace for the first mile. Running backwards during your first mile is also a very effective way to warm up the Achilles, because doing so produces a gentle eccentric load that acts to strengthen the tendon. Runners should also avoid making sudden changes in mileage, and they should be particularly careful when wearing racing flats, as these shoes produce very rapid rates of pronation that increase the risk of Achilles tendon injury. If you have a tendency to be stiff, spend extra time stretching. If you?re overly flexible, perform eccentric load exercises preventively. Lastly, it is always important to control biomechanical alignment issues, either with proper running shoes and if necessary, stock or custom orthotics.
What Is Pes Planus?

he belly isn't the only part of your body subject to middle-age spread. As we get older, the years of walking and standing can cause feet to spread and flatten out as ligaments that support the arch lose their holding power. The result: the condition known as fallen arches, or flat feet. "Keep in mind that we're talking about 26 bones in the foot that are supported by a series of ligaments, muscle tendons and other connective tissue," says Glenn Gastwirth, D.P.M., deputy executive director of the American Podiatric Medicine Association in Bethesda, Maryland. "Over a period of time, the ligaments stretch out or 'give' under the pressure of your weight-especially if you're overweight. So what usually happens is you go shopping for new shoes one day and suddenly realize that you now need a size 8 when you've always worn a size 6. You may think your foot has grown, but what really happens is that the foot has spread out, both in width and length."
Causes
There are several factors that can contribute to the development of fallen arches. These factors include the following. Genetic abnormality, torn or stretched tendons, amage to the posterior tibial tendon, bone fractures, dislocation of bones, nerve damage, rheumatoid arthritis and other medical conditions. In addition, there are other factors that can increase your risk of developing fallen arches. These risk factors include diabetes, pregnancy, Obesity and Aging.
Symptoms
The majority of children and adults with flexible flatfeet never have symptoms. However, their toes may tend to point outward as they walk, a condition called out-toeing. A person who develops symptoms usually complains of tired, aching feet, especially after prolonged standing or walking. Symptoms of rigid flatfoot vary depending on the cause of the foot problem. Congenital vertical talus. The foot of a newborn with congenital vertical talus typically has a convex rocker-bottom shape. This is sometimes combined with an actual fold in the middle of the foot. The rare person who is diagnosed at an older age often has a "peg-leg" gait, poor balance and heavy calluses on the soles where the arch would normally be. If a child with congenital vertical talus has a genetic disorder, additional symptoms often are seen in other parts of the body. Tarsal coalition. Many people have no symptoms, and the condition is discovered only by chance when an X-ray of the foot is obtained for some other problem. When symptoms occur, there is usually foot pain that begins at the outside rear of the foot. The pain tends to spread upward to the outer ankle and to the outside portion of the lower leg. Symptoms usually start during a child's teenage years and are aggravated by playing sports or walking on uneven ground. In some cases, the condition is discovered when a child is evaluated for unusually frequent ankle sprains. Lateral subtalar dislocation. Because this often is caused by a traumatic, high-impact injury, the foot may be significantly swollen and deformed. There also may be an open wound with bruising and bleeding.
Diagnosis
People who have flat feet without signs or symptoms that bother them do not generally have to see a doctor or podiatrist about them. However, if any of the following occur, you should see your GP or a podiatrist. The fallen arches (flat feet) have developed recently. You experience pain in your feet, ankles or lower limbs. Your unpleasant symptoms do not improve with supportive, well-fitted shoes. Either or both feet are becoming flatter. Your feet feel rigid (stiff). Your feet feel heavy and unwieldy. Most qualified health care professionals can diagnose flat feet just by watching the patient stand, walk and examining his/her feet. A doctor will also look at the patient's medical history. The feet will be observed from the front and back. The patient may be asked to stand on tip-toe while the doctor examines the shape and functioning of each foot. In some cases the physician may order an X-ray, CT (computed tomography) scan, or MRI (magnetic resonance imaging) scan.
Non Surgical Treatment
The treatment is simple for flat feet. We will carry out a biomechanical assessment and full history, often along side a Computerised Gait Scan to give us an idea of how the foot is compensating. Treatment will be to, control how the foot hits the ground, support the middle of the foot and prevent the arch collapsing, promote normal movement in the front of the foot. The ability to do this will be dictated by the movement within the foot to start with. Treatment for all the above problems are often combined with a physiotherapy session in order to help develop a stretching and strengthening program for the back of the legs and the pelvis in order to allow normal function when the orthoses have been prescribed. If you are born with flat feet you will not grow out of them - if you get orthoses, like glasses you will need them for the rest of your life if you want to correct the mechanics in your foot. In 95% of cases, orthoses will reduce symptoms by at least 85%. In the other 5% we will work with them to get them to this level.
Surgical Treatment

Fallen arches may occur with deformities of the foot bones. Tarsal coalition is a congenital condition in which the bones of the foot do not separate from one another during development in the womb. A child with tarsal coalition exhibits a rigid flat foot, which can be painful, notes the patient information website eOrthopod. Surgery may prove necessary to separate the bones. Other foot and ankle conditions that cause fallen arches may also require surgery if noninvasive treatments fail to alleviate pain and restore normal function.
Prevention
Going barefoot, particularly over terrain such as a beach where muscles are given a good workout, is good for all but the most extremely flatfooted, or those with certain related conditions such as plantar fasciitis. Ligament laxity is also among the factors known to be associated with flat feet. One medical study in India with a large sample size of children who had grown up wearing shoes and others going barefoot found that the longitudinal arches of the bare footers were generally strongest and highest as a group, and that flat feet were less common in children who had grown up wearing sandals or slippers than among those who had worn closed-toe shoes. Focusing on the influence of footwear on the prevalence of pes planus, the cross-sectional study performed on children noted that wearing shoes throughout early childhood can be detrimental to the development of a normal or a high medial longitudinal arch. The vulnerability for flat foot among shoe-wearing children increases if the child has an associated ligament laxity condition. The results of the study suggest that children be encouraged to play barefooted on various surfaces of terrain and that slippers and sandals are less harmful compared to closed-toe shoes. It appeared that closed-toe shoes greatly inhibited the development of the arch of the foot more so than slippers or sandals. This conclusion may be a result of the notion that intrinsic muscle activity of the arch is required to prevent slippers and sandals from falling off the child?s foot.
Pain In The Arches Causes Symptoms And Treatments
Arch pain is the term used to describe pin under the arch of the foot. Arch pain is common in people with flat feet. When this occurs it means the person has some inflammation in the mid foot. The arch is supported by a tight band of tissue called the Planter fascia, running from the toes to the heel bone. When this is inflamed it is known as Plantar Fasciitis.

Causes
Often, tarsal tunnel syndrome is misdiagnosed and confused with plantar fasciitis. Tarsal tunnel syndrome is when the tibial nerve which runs through the ankle, is pinched as it passes through the flexor retinaculum, the supportive band that surrounds the ankle joint. The symptoms of tarsal tunnel syndrome are often limited to the ankle but the since the nerve passes through the entire foot it can cause arch pain. Arch pain associated with foot strain is mainly caused by a pronated foot (rolls inward) or a flat foot. These are usually not singular causes of arch pain, but in combination with other factors, arch pain may result.
Symptoms
The primary symptom is pain or aching in the arch area. This can be accompanied by inflammation and tenderness. If the pain is caused by the plantar fascia, it is likely to be considerably more severe in the mornings due to the muscles being unused.
Diagnosis
The doctor will take a brief history to determine how the injury occurred. If necessary, a thorough physical exam may be conducted to evaluate for any other injuries. Taking your workout shoes to the exam may also provide valuable information to the medical practitioner. Both feet will be physically and visually examined by the medical practitioner. The foot and arch will be touched and manipulated possibly with a lot of pressure and inspected to identify obvious deformities, tender spots, or any differences in the bones of the foot and arch.
Non Surgical Treatment
More than 90% of patients with plantar fasciitis will improve within 10 months of starting simple treatment methods. Rest. Decreasing or even stopping the activities that make the pain worse is the first step in reducing the pain. You may need to stop athletic activities where your feet pound on hard surfaces (for example, running or step aerobics). Ice. Rolling your foot over a cold water bottle or ice for 20 minutes is effective. This can be done 3 to 4 times a day. Nonsteroidal anti-inflammatory medication. Drugs such as ibuprofen or naproxen reduce pain and inflammation. Using the medication for more than 1 month should be reviewed with your primary care doctor. Exercise. Plantar fasciitis is aggravated by tight muscles in your feet and calves. Stretching your calves and plantar fascia is the most effective way to relieve the pain that comes with this condition.

Surgical Treatment
Surgery is considered only after 12 months of aggressive nonsurgical treatment. Gastrocnemius recession. This is a surgical lengthening of the calf (gastrocnemius) muscles. Because tight calf muscles place increased stress on the plantar fascia, this procedure is useful for patients who still have difficulty flexing their feet, despite a year of calf stretches. In gastrocnemius recession, one of the two muscles that make up the calf is lengthened to increase the motion of the ankle. The procedure can be performed with a traditional, open incision or with a smaller incision and an endoscope, an instrument that contains a small camera. Your doctor will discuss the procedure that best meets your needs. Complication rates for gastrocnemius recession are low, but can include nerve damage. Plantar fascia release. If you have a normal range of ankle motion and continued heel pain, your doctor may recommend a partial release procedure. During surgery, the plantar fascia ligament is partially cut to relieve tension in the tissue. If you have a large bone spur, it will be removed, as well. Although the surgery can be performed endoscopically, it is more difficult than with an open incision. In addition, endoscopy has a higher risk of nerve damage. The most common complications of release surgery include incomplete relief of pain and nerve damage. Most patients have good results from surgery. However, because surgery can result in chronic pain and dissatisfaction, it is recommended only after all nonsurgical measures have been exhausted.
Prevention
The best way to prevent plantar fasciitis is to wear shoes that are well made and fit your feet. This is especially important when you exercise, walk a lot, or stand for a long time on hard surfaces. Get new athletic shoes before your old shoes stop supporting and cushioning your feet. You should also avoid repeated jarring to the heel. Maintain a healthy weight. Stretch when you feel a tightening of the ligament that runs along the bottom of your foot. Stop impact sports when symptoms first occur.
Stretching Exercises
Gastroc stretch. Stand on the edge of a step. Rise slowly on your toes. Lower yourself slowly as far as you can until you feel a stretch in your calf. Don?t roll your foot inward or outward. Hold for 1-2 seconds. Reps:10-20 (stop before you fatigue). Soleus stretch. Same as above, but start with your knee bent so that you feel a slight stretch in your calf or achilles. Maintain the angle of your knee throughout the stretch. Bicycle stretch. Lie on your side. Keeping your top leg straight, bring your knee toward your nose until you feel a slight stretch in the hamstring. Maintaining this angle at your hip, start pretending you are pedalling a bicycle with the top leg. Make sure you feel a slight stretch each time your knee is straight. Reps: 10-30 for each leg. If you feel any pops or clicks in your hip or back, try raising the top leg a little (making the thighs further apart) to eliminate the popping. Foot Intrinsic Exercises. Assisted metatarsal head raising. Sit in a chair. Find the bumps at the ball of your foot just before your big toe and just before the little toe. These are the first (big toe) and fifth (little toe) metatarsal heads. Place your second and third fingers from one hand under the first metatarsal head, and the second and third fingers from the other hand under the fifth metatarsal head. Now lay the thumbs from each hand in a diagonal across your toes so that they form a right angle meeting at the nail of the second toe. Your hands are now in position to assist your toes. Keep your toes straight, with the toe pads on the floor. Use your fingers to help raise all the metatarsal heads (the ball of your foot). Do not let your toes curl under keep them long. Now relax. Reps 7-10 for each foot. As this exercise gets easier, let your fingers do less of the work until your toes can do the exercise unassisted. This can take up to three weeks. When your strength has improved to this point, you can progress to the following three exercises, which are best done in stocking feet on a slippery floor. Active metatarsal head raising. Stand with your weight on both feet. Raise your metatarsal heads (the ball of your foot) while keeping your toes from curling under and maintaining your heel on the ground. Relax. Reps 6-7. Do one foot at a time. If you do more reps than you are ready for, you may well develop cramping in your foot. I once had a client who thought if seven reps were good, 10 were better. For good measure, she did the 10 reps 10 times in a day, and then she was unable to walk the next day from having used a set of muscles she had never exercised before. Don?t overdo it.
The Cause For Adult Aquired Flat Feet
A painful flat foot, or perhaps adult acquired flatfoot deformity, can be a progressive collapsing of the arch with the foot that develops as the posterior tibial tendon gets in order to be insufficient due to numerous factors. Early stages might existing using simply pain along the posterior tibial tendon whereas advanced deformity generally leads to arthritis along with rigidity with the rearfoot and ankle.

Causes
Causes involving a grown-up acquired flatfoot might include Neuropathic foot (Charcot foot) secondary for you to Diabetes mellitus, Leprosy, Profound peripheral neuritis involving just about any cause. Degenerative changes in the ankle, talonavicular or even tarsometatarsal joints, or even both, secondary to end up being able to Inflammatory arthropathy, Osteoarthropathy, Fractures, Acquired flatfoot resulting coming from loss with the supporting structures with the medial longitudinal arch. Dysfunction in the tibialis posterior tendon Tear with the spring (calcaneoanvicular) ligament (rare). Tibialis anterior rupture (rare). Painful flatfoot can easily have got some other causes, such as tarsal coalition, however as this sort of patient will not existing using a adjust within the model of the actual foot these aren't included here.
Symptoms
Your feet tire effortlessly as well as become painful using prolonged standing. It's difficult to go your own heel as well as midfoot around, in order to stand in your toes. Your Own foot aches, particularly inside the heel or arch area, using swelling across the inner side. Pain inside your feet reduces the power to participate in sports. You've been clinically established to become able to have rheumatoid arthritis; concerning 1 / 2 of all people that have rheumatoid arthritis will develop a new progressive flatfoot deformity.
Diagnosis
The background and physical examination are probably one of the most essential tools the particular physician makes use of for you to diagnose this problem. The Actual put on pattern on your own shoes can provide some useful clues. muscle screening helps identify virtually any places of weakness or perhaps muscle mass impairment. This specific ought to be completed throughout both the weight bearing and also nonweight bearing positions. a very effective test will become the single heel raise. Anyone will probably be inspired to get up on one foot and arise on your toes. you should be in a place to lift your heel up and also running easily although trying for you to keep the particular calcaneus (heel bone) within the middle together with slight inversion (turned inward). X-rays are often utilized to research the position, shape, and also alignment with the bones in the feet and ankles. Magnetic resonance (MR) imaging is the imaging modality of choice regarding evaluating the posterior tibial tendon as well as spring ligament complex.
Non surgical Treatment
Orthotic or perhaps anklebrace, Over-the-counter as well as custom shoe inserts to situation the foot and also relieve pain are one of the most typical non-surgical remedy option. Custom orthotics are often suggested when the shape alter in the foot is a excellent deal more severe. An ankle brace (either over-the-counter or perhaps custom made) is an additional alternative that may assistance to ease tendon tension and also pain. Boot immobilization. Any strolling boot props up tendon and also allows it for you to heal. activity modifications. Depending on which we find, organic beef recommend limiting high-impact activities, such as running, jumping or perhaps court sports, or switching out high-impact activities with regard to low-impact choices to find a time period regarding time. Ice along with anti-inflammatory medications. These types of may end up being given as necessary to decrease the symptoms.
Surgical Treatment
In case conservative treatment method fails surgical intervention can be offered. With Regard To any Stage one deformity a new posterior tibial tendon tenosynovectomy (debridement in the tendon) as well as primary repair could become indicated. With Regard To Stage two a mixture of Achilles lengthening with bone cuts, calcaneal osteotomies, as well as tendon transfers will be common. Stage two versatile PTTD may end up being the most typical stage patients existing along with pertaining to treatment. Inside Stage three as well as 4 PTTD isolated fusions, locking a couple of or even a lot more joints together, maybe indicated. all treatment method depends about the stage as well as severity with presentation with the goals and also exercise amount patient throughout mind. Therapy will be customized to the individual individual needs.
Pain In The Arch Triggers Symptoms And Treatment Plans
A cavus or high-arched foot may have many foot shapes. This may range from an arch that is slightly high to a severe deformity that causes a patient to walk on the outside of the foot. Surgery is occasionally required to realign the foot. There are different causes of a high-arched foot. In many cases, the cause is unknown. In other cases, the cause is a nerve disease, clubfoot or injury. Treatment ranges from changes in shoewear to surgeries, depending on the amount of deformity and related problems.

Causes
Training on improper, hard and/or irregular surfaces as well as excessive track work in spiked shoes, or steep hill running, can stress the plantar fascia past its limits of elasticity, leading to injury. Finally, failure in the early season to warm up gradually gives the athlete insufficient time for the structures of the foot to re-acclimate and return to a proper fitness level for intensive exercise. Such unprepared and repeated trauma causes microscopic tearing, which may only be detected once full-blown plantar fasciitis and accompanying pain and debilitation have resulted.
Symptoms
Arch pain may have a variety of different causes. Proper evaluation and diagnosis of arch pain is essential in planning treatment. A good general guideline is to compare the injured side to the uninjured side. Injury may present itself as a distinguishable lump, a gap felt at that location, or a "crunchy" feeling on that spot caused by inflammation. The type, causes, and severity of pain are also good indicators of the severity of the injury.
Diagnosis
The adult acquired flatfoot, secondary to posterior tibial tendon dysfunction, is diagnosed in a number of ways with no single test proven to be totally reliable. The most accurate diagnosis is made by a skilled clinician utilizing observation and hands on evaluation of the foot and ankle. Observation of the foot in a walking examination is most reliable. The affected foot appears more pronated and deformed compared to the unaffected foot. Muscle testing will show a strength deficit. An easy test to perform in the office is the single foot raise.
Non Surgical Treatment
Depending on your overall health, symptoms and severity of the the flat foot, the condition may be treated conservatively and/or with surgery. Non-surgical treatments for flat feet are centered at decreasing and/or resolving the symptoms (pain). Simple Treatments Patients Can do themselves include wear proper supportive shoes. Use an arch support. Wear shoes with a wide toe box. Modify your activities. Lose weight. Wear shoes with cushion. Non-surgical treatments a doctor might do include Prescribe an oral anti-inflammatory medication. Anti-inflammatory medication is useful to significantly reduce pain and inflammation. Prescribe physical therapy. A physical therapist may perform ultrasound and other techniques to reduce inflammation. You will also be instructed how to stretch your foot and leg properly. Keeping the joint mobile may preserve function. Strengthening weak foot and leg musculature can help prevent further collapse. Prescribe protective pads. Padding and/or cushioning of when areas of bone become prominent on the bottom of the foot, as an effective method of preventing mechanical irritation with shoes. Pads with cutouts may off-weight specific areas of concern. Prescribe custom foot orthotics. A custom foot orthotic is a doctor prescribed arch support that is made directly from a casting (mold) of your feet, and theoretically should provide superior support compared to shoe insert that you would purchase from a pharmacy. In the case of flat feet, specific modifications can be made to the orthotic device to strategically balance the foot. Prescribe custom ankle-foot orthoses. A custom ankle-foot orthotic (AFO) is a doctor prescribed molded arch and lower leg support that stabilizes both the foot and ankle. This is used when the flat foot is significant and provides more support than the simple foot only insert. Give cortisone injection. A articular cortisone injection is a powerful anti-inflammatory medication that is used to rapidly reduce the pain associated with inflammation. Cortisone shots can be extremely effective in alleviating symptoms of flat feet, but will not correct the structure.

Surgical Treatment
Surgical advances have dramatically improved the ability to alleviate the pain and decreased function that millions of Americans experience due to flat feet. Nevertheless, many patients and even some physicians remain unaware of the new procedures, which are best performed by a foot and ankle specialist who has the applicable training and experience.
Prevention
Stretch and strengthen important muscles in your feet, ankles and legs in order to guard against future strain. Make sure to acquire suitable arch supports and inserts if necessary, and that your shoes are shock absorbent and in good condition. Wearing tattered shoes provides no protection, and runners should replace their footwear before exceeding 500 miles of usage. Athletes new to arch supports should gradually build their training routine, allowing their feet to become accustomed to a new stance.
Stretching Exercises
Below are two simple plantar fasciitis stretching exercises to help improve the flexibility of the muscles and tendons around the foot and ankle. Plantar fasciitis stretch taken from The Stretching Handbook. Kneel on one foot and place your body weight over your knee. Keep your heel on the ground and lean forward. In the photo to the left, the athlete is stretching the arch of her left foot. Kneel on one foot with your hands on the ground. Place your body weight over your knee and slowly move your knee forward. Keep your toes on the ground and arch your foot. In the photo to the right, the athlete is stretching the arch of his right foot.
Pain In The Arch What Are The Causes ?
Flexible flatfeet are considered normal in young children because babies are not born with a normal arch. The arch may not form fully until sometime between ages 7 and 10. Even in adulthood, 15% to 25% of people have flexible flatfeet. Most of these people never develop symptoms. In many adults who have had flexible flatfeet since childhood, the missing arch is an inherited condition related to a general looseness of ligaments. These people usually have extremely flexible, very mobile joints throughout the body, not only in the feet. Flatfeet also can develop during adulthood. Causes include joint disease, such as rheumatoid arthritis, and disorders of nerve function (neuropathy).

Causes
There are many causes for a high arch (cavus) foot. In the United States, the most common cause for a high arch foot is a form of muscular dystrophy called hereditary sensorimotor neuropathy. Most people recognize this by the more commonly used name of Charcot Marie Tooth disease (CMT). This is a disease of the muscles and the nerves of the legs, and occasionally of the hands, in which certain muscles weaken while others retain their strength. The condition is transmitted as an autosomal dominant condition. This means that 50% of the offspring will statistically inherit the disorder. This is, however, just a statistic. In some families, all the children develop the condition while in others, none inherit it.
Symptoms
Bones and ligaments work together to form joints, and bones are joined together by ligaments. Strains occur in ligaments. In the arch, there are ligaments that are located at the ends of each bone. These ligaments connect the bones to other bones on both ends and on the sides. Point tenderness and looseness of a joint are indicators of a sprain. Fractures are indicated by point tenderness that may be severe over the area of bone that is affected. There may be a distinguishable lump or gap at the site of the fracture. A rotated toe or forefoot may also be a sign of a fracture.
Diagnosis
The doctor will take a brief history to determine how the injury occurred. If necessary, a thorough physical exam may be conducted to evaluate for any other injuries. Taking your workout shoes to the exam may also provide valuable information to the medical practitioner. Both feet will be physically and visually examined by the medical practitioner. The foot and arch will be touched and manipulated possibly with a lot of pressure and inspected to identify obvious deformities, tender spots, or any differences in the bones of the foot and arch.
Non Surgical Treatment
Though most FFF are asymptomatic (no pain or discomfort), they should still be addressed as it is not normal to have flat feet. Obviously it is always ideal to prevent a problem rather than treat it after it occurs, especially if FFF is being treated post-foot development. As mentioned earlier, barefoot is the best way to prevent FFF and a host of other foot and gait imbalances. To truly strengthen the entire foot and all the arches, it?s important to position the foot correctly at all times so when wearing something on the feet, footwear should be flat, firm, and flexible. This means that the shoe should not have a significant, or any, heel to toe drop, there should be little to no cushion or padding in the sole, and the shoe should not be rigid anywhere - it should bend throughout the shoe and in any direction. The shoe should also be wide at the toe box allowing the toes to naturally splay apart.

Surgical Treatment
The main goal of surgery is to reduce pain and improve function. It may also reduce other injuries such as repeated ankle sprains and broken bones. Surgery may be considered if there is no relief with physical therapy, changes in shoewear and/or changes in activity. Some patients will also have tendon problems, ankle weakness and foot fractures. These patients may require other procedures to address related problems. If you have medical problems that make surgery unsafe, any infections or blood vessel disease, cavus foot surgery may not be appropriate. The surgical procedures involved with the correction of the cavus foot are varied. Theses may include correction of the bony deformity, ankle looseness and the muscle imbalances that cause the deformity. The goal is to provide a foot that evenly distributes weight along both inside and outside edges. A variety of incisions may be needed to perform the procedures related to the correction of the cavus foot.
Stretching Exercises
Achilles stretch. Stand with the ball of one foot on a stair. Reach for the step below with your heel until you feel a stretch in the arch of your foot. Hold this position for 15 to 30 seconds and then relax. Repeat 3 times. Balance and reach exercises. Stand next to a chair with your injured leg farther from the chair. The chair will provide support if you need it. Stand on the foot of your injured leg and bend your knee slightly. Try to raise the arch of this foot while keeping your big toe on the floor. Keep your foot in this position. With the hand that is farther away from the chair, reach forward in front of you by bending at the waist. Avoid bending your knee any more as you do this. Repeat this 15 times. To make the exercise more challenging, reach farther in front of you. Do 2 sets of 15. While keeping your arch raised, reach the hand that is farther away from the chair across your body toward the chair. The farther you reach, the more challenging the exercise. Do 2 sets of 15. Towel pickup. With your heel on the ground, pick up a towel with your toes. Release. Repeat 10 to 20 times. When this gets easy, add more resistance by placing a book or small weight on the towel. Resisted ankle plantar flexion. Sit with your injured leg stretched out in front of you. Loop the tubing around the ball of your foot. Hold the ends of the tubing with both hands. Gently press the ball of your foot down and point your toes, stretching the tubing. Return to the starting position. Do 2 sets of 15. Resisted ankle dorsiflexion. Tie a knot in one end of the elastic tubing and shut the knot in a door. Tie a loop in the other end of the tubing and put the foot on your injured side through the loop so that the tubing goes around the top of the foot. Sit facing the door with your injured leg straight out in front of you. Move away from the door until there is tension in the tubing. Keeping your leg straight, pull the top of your foot toward your body, stretching the tubing. Slowly return to the starting position. Do 2 sets of 15. Heel raise. Stand behind a chair or counter with both feet flat on the floor. Using the chair or counter as a support, rise up onto your toes and hold for 5 seconds. Then slowly lower yourself down without holding onto the support. (It's OK to keep holding onto the support if you need to.) When this exercise becomes less painful, try doing this exercise while you are standing on the injured leg only. Repeat 15 times. Do 2 sets of 15. Rest 30 seconds between sets.